The Drug That’s Being Used To Combat ‘Brain-Eating Amoeba’ In Kerala
Kerala is facing a rare but deadly health challenge—Primary Amoebic Meningoencephalitis (PAM), a brain infection caused by Naegleria fowleri, widely known as the “brain-eating amoeba.” Globally, this infection carries a mortality rate of more than 95%, leaving only a handful of survivors worldwide.
Yet, in 2025, Kerala has shown remarkable improvement. Out of nearly 70 reported PAM cases this year, the state has achieved a 24% survival rate, far higher than the global average of under 3%.
One major factor behind this success is the use of miltefosine, an antiparasitic drug now added to Kerala’s treatment protocol for suspected PAM cases. Combined with early diagnosis, rapid medical response, and rigorous supportive care, this drug has helped tilt the balance in favor of survival in a disease that usually kills within days.
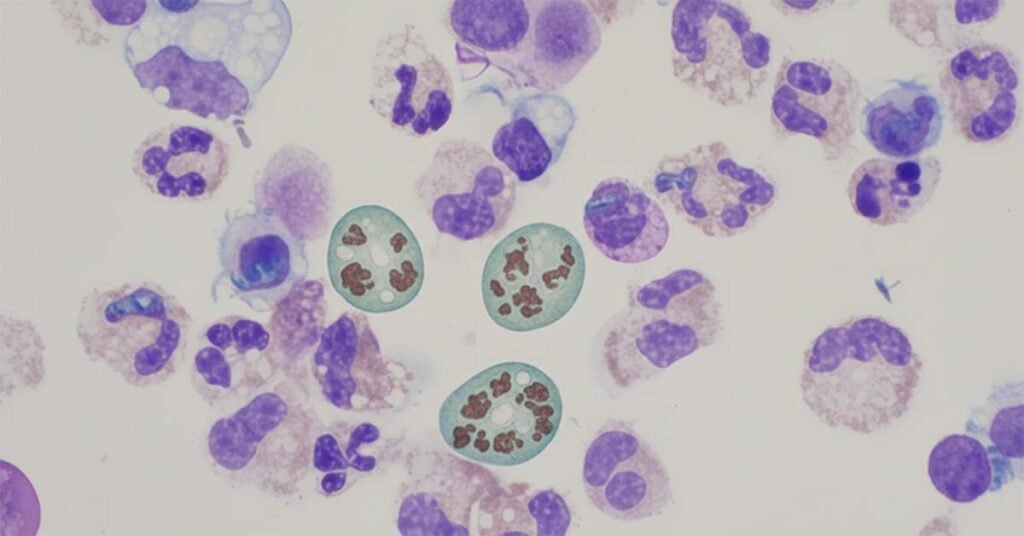
What Makes PAM So Deadly?
PAM occurs when Naegleria fowleri enters the human body through the nose, usually during swimming or bathing in warm freshwater. From there, it travels to the brain, causing severe inflammation.
| Key Fact | Details |
|---|---|
| Fatality Rate | More than 97% globally |
| Time to Death | Usually 5–10 days after symptoms begin |
| Early Symptoms | Fever, headache, nausea, stiff neck, confusion |
| Later Symptoms | Seizures, coma, and death |
Because PAM resembles bacterial or viral meningitis, diagnosis is often delayed. By the time doctors recognize it, the infection is usually too advanced. Kerala’s approach of early recognition and immediate therapy has proven critical.
Kerala’s Improved Survival Rate
In most parts of the world, PAM has remained almost uniformly fatal. In the U.S., for example, only a handful of patients have ever survived despite aggressive treatment.
But in Kerala, survival has risen to nearly one in four patients. Doctors at Kozhikode Medical College Hospital credit this to:
-
Faster lab testing and heightened clinical suspicion of PAM
-
Starting anti-amoebic therapy within hours of admission
-
Using miltefosine in combination with amphotericin B and other drugs
-
Advanced ICU care to manage brain swelling and seizures
Recently, an 11-year-old girl from Malappuram was discharged after testing negative for the amoeba twice in 15 days, making her one of four survivors in Kozhikode within weeks. Recoveries like this would have been almost unthinkable a decade ago.
Miltefosine: The Drug Making a Difference
What is miltefosine?
Miltefosine is an oral antiparasitic drug. Originally developed as an anti-cancer treatment, it later became a frontline medicine for leishmaniasis, a parasitic disease spread by sandflies.
Researchers later discovered that miltefosine is also effective against free-living amoebae, including Naegleria fowleri. Its ability to disrupt cell membranes and signaling pathways gave doctors hope that it could help in PAM cases.
Evolution of miltefosine use:
-
Cancer research: Initially tested as an anti-tumor drug
-
Leishmaniasis: Approved and widely used in India and other endemic regions
-
Brain infections: Now used in rare cases of PAM and Acanthamoeba keratitis
How Kerala Uses Miltefosine in PAM Treatment
There is no global standard for PAM therapy. Treatment usually involves multiple drugs, ICU care, and physician judgment.
| Treatment Component | Details |
|---|---|
| Amphotericin B | Intravenous; sometimes intrathecal (directly into CSF) |
| Miltefosine | Oral, started early in suspected cases |
| Azoles | Fluconazole or Voriconazole |
| Rifampin | Used in selected cases |
| ICU Supportive Care | Monitoring of brain pressure, ventilatory and fluid support |
| Adult Dosage (>45 kg) | Miltefosine 50 mg three times daily with food |
| Child Dosage (<45 kg) | Miltefosine 50 mg twice daily, adjusted by weight |
| Treatment Duration | At least 28 days, adjusted based on recovery and clinical response |
Doctors emphasize that starting miltefosine as soon as PAM is suspected—even before lab confirmation—can make a difference.
Why Miltefosine May Be Helping Kerala
Kerala’s improved outcomes can be linked to:
-
Earlier diagnosis due to better awareness among doctors
-
Aggressive combination therapy (miltefosine + amphotericin B + others)
-
Improved ICU care for brain swelling and seizures
-
Public health awareness campaigns about freshwater safety
While miltefosine is not a guaranteed cure, it clearly improves survival odds when started early.
Risks and Side Effects of Miltefosine
Like all strong drugs, miltefosine carries risks.
| Category | Details |
|---|---|
| Common Side Effects | Nausea and vomitingDiarrheaAbdominal painFatigue |
| Serious Risks | Kidney and liver function changesElectrolyte imbalancesReproductive risks (not recommended during pregnancy unless life-saving) |
Because PAM patients are critically ill, doctors must weigh these risks against the near-certain fatality without treatment.
Limitations of Current Knowledge
Despite Kerala’s promising results, challenges remain:
-
No large clinical trials proving miltefosine’s effectiveness in PAM
-
Most data comes from small case reports
-
Limited drug availability in some hospitals
-
Survival, while improved, is still not guaranteed
This is why prevention remains as important as treatment.
Public Health Measures in Kerala
Kerala has paired drug treatment with prevention efforts:
-
Chlorination of public water bodies
-
Advisories against swimming in untreated ponds and rivers
-
Guidance on safe nasal rinsing (only with boiled, cooled, or distilled water)
-
Training doctors to spot PAM symptoms early
These measures aim to both reduce new infections and improve outcomes.
Key Takeaways
-
Brain-eating amoeba infections (PAM) are rare but deadly, with global survival under 3%.
-
Kerala’s survival rate has improved to 24%, thanks to early detection, ICU care, and miltefosine use.
-
Miltefosine is not a cure, but it improves survival chances when used in combination therapy.
-
Treatment requires strict hospital monitoring due to side effects.
-
Prevention is the best protection—through safe water practices and avoiding untreated freshwater exposure.
Conclusion
The rise in PAM cases in Kerala has brought the “brain-eating amoeba” into sharp focus. While the infection remains rare, its deadly nature makes every recovery significant.
The introduction of miltefosine into Kerala’s treatment protocol marks a small but vital breakthrough—raising survival rates where previously there was almost no hope.
For families and doctors, miltefosine is not a miracle cure, but it is now an essential tool in the fight against this deadly amoeba. The world will be watching Kerala’s approach closely in the years to come.
Frequently Asked Questions (FAQ)
1. What is the brain-eating amoeba?
The brain-eating amoeba is Naegleria fowleri, a microscopic organism that lives in warm freshwater. It causes Primary Amoebic Meningoencephalitis (PAM), a rare but usually fatal brain infection.
2. How does a person get infected with Naegleria fowleri?
Infection occurs when contaminated water enters the nose, usually during swimming or bathing in untreated ponds, rivers, or lakes. The amoeba then travels to the brain and causes inflammation. It cannot infect people through drinking water.
3. What are the early symptoms of PAM?
Early symptoms appear 1–7 days after exposure and include:
-
Severe headache
-
Fever
-
Nausea or vomiting
-
Stiff neck
-
Confusion
As the infection progresses, symptoms may worsen to seizures, coma, and eventually death.
4. How is PAM treated in Kerala?
Kerala follows a combination therapy protocol that includes:
-
Amphotericin B (injected into the vein or spinal fluid)
-
Miltefosine (oral drug started early)
-
Azoles (fluconazole or voriconazole)
-
ICU supportive care to manage brain swelling and seizures
5. Why is miltefosine important in treating brain-eating amoeba?
Miltefosine is an antiparasitic drug that disrupts amoeba cell membranes. While not a cure, it improves survival when used alongside amphotericin B and other medicines. In Kerala, early use of miltefosine has helped raise PAM survival rates to nearly 24%, compared to less than 3% globally.
6. Can PAM be prevented?
Yes. Prevention is the most effective protection against PAM:
-
Avoid swimming in untreated warm freshwater ponds and rivers.
-
Use only boiled, cooled, or distilled water for nasal rinsing (e.g., neti pot).
-
Ensure proper chlorination of swimming pools and water tanks.
7. What is the survival rate of PAM in Kerala compared to the world?
Globally, PAM has a survival rate of less than 3%. In Kerala, thanks to early diagnosis, miltefosine therapy, and improved ICU care, survival has improved to about 24% in 2025.